A prescription that says “take 3 times a day” may look simple, but the timing often cause confusion. Many people know they need three doses. They just do not know the best hours to place them. One dose can end up too close to the next, or the last dose can move too far into the evening. That kind of spacing can make the schedule less reliable and harder to maintain.
A clear plan starts with the right interval between doses. After that, it becomes much easier to choose times that fit your normal day. Meals, work, and sleep matter here. This is the step that usually creates the most questions.
The label gives the instruction, but it does not always explain how to turn that instruction into a practical daily routine. Your prescription label and pharmacist directions come first if they differ from general schedules.
Pick the gap first, then pick the times
People often pick three “convenient” times and call it a plan. That is where timing problems start. The gaps become uneven, and the routine feels harder to follow. Start with the space between doses. Many medicines work best when you keep the gaps steady. Three doses across a full day usually works out to about 8 hours apart. That is why some labels say “every 8 hours,” and antibiotics often follow that rule.
Real life can work differently. Most people stay awake about 14 to 16 hours. Some medicines allow you to place three doses across your waking hours instead of using a strict 24-hour cycle.
Some labels expect strict 8-hour gaps across a full 24-hour cycle. Other labels allow three doses during waking hours. The right option depends on your directions and how strict the timing needs to be. The other spreads three doses evenly during the hours you are awake. The right option depends on your label directions and how strict the timing needs to be.
Use times you can repeat on busy days
A schedule can look correct and still fail in real life. The reason is simple. People miss doses when the plan does not match how they actually live. A good plan should feel easy to repeat on busy days, not just on quiet days.

Pick a routine you can keep without stress. Most people do best when they tie doses to the same daily anchors. Meals and sleep work well as anchors. This turns medicine timing into a habit, not a constant clock check.
A practical day often follows this flow:
- First dose near breakfast
- Second dose in the afternoon
- Third dose in the evening
This pattern keeps the day smooth. It also reduces the chance of late-night alarms.
Here is a simple example that fits many schedules:
- 8 AM
- 2 PM
- 8 PM
It works because it matches normal daily hours. You do not need to wake up very early or stay up very late to follow it.
A later start can also work well. Keep the gaps steady and choose times you can repeat daily:
- 10 AM
- 4 PM
- 10 PM
The exact times can shift based on your routine. Steady spacing matters more than perfect math.
Schedules You Can Copy Today
| Your day starts around | Dose 1 | Dose 2 | Dose 3 | Notes |
|---|---|---|---|---|
| Early routine | 7:00 AM | 1:00 PM | 7:00 PM | Simple daytime rhythm |
| Standard routine | 8:00 AM | 2:00 PM | 8:00 PM | Most common and repeatable |
| Late routine | 10:00 AM | 4:00 PM | 10:00 PM | Works if label allows waking-hours timing |
When you can’t ‘adjust’ the schedule
Sometimes your routine cannot control the schedule. The medicine sets the rules. This happens most often with antibiotics and other drugs that must stay at a steady level in your body.
In these cases, the main goal is even spacing. A loose schedule can reduce the effect of the medicine. It can also make treatment less reliable.
A strict three-times-a-day plan often uses near 8-hour gaps, such as:
- 6 AM
- 2 PM
- 10 PM
This pattern repeats each day. It does not shift just because you sleep late or wake up early.
Night or early morning doses can feel inconvenient. Many people still need alarms or reminders to stay on track. That effort matters because it helps the medicine work the way your doctor intended.
3x daily isn’t always every 8 hours
| Label wording | What it usually means | How strict is timing | Example schedule |
|---|---|---|---|
| 3 times daily (TID) | 3 doses during the day | Often flexible | 8 AM / 2 PM / 8 PM |
| Every 8 hours (Q8H) | Keep 8-hour gaps across 24 hours | Strict | 6 AM / 2 PM / 10 PM |
| Strict spacing needed | Medicine needs steady level | Very strict | May include night dose |
Many people treat these two instructions as the same. They are not the same. The difference affects your whole schedule. 3 times daily often means three doses during the day. This usually allows some flexibility. You still want steady spacing, but the plan can fit your normal waking hours.
Every 8 hours is more strict. It means you keep the gap close to 8 hours no matter what time you wake up or go to sleep. This instruction often appears on antibiotics and other medicines that need steady levels in the body. A quick way to remember it is simple.
Three times daily can adapt to your day. Every 8 hours does not adapt to your day. It follows the medicine. If your label feels unclear, confirm with a pharmacist. One small misunderstanding can lead to missed doses or uneven spacing.
The 1:52 PM example that surprises people
Here is a simple case. You take your first dose at 1:52 PM. You decide to follow strict spacing. You add 8 hours each time.
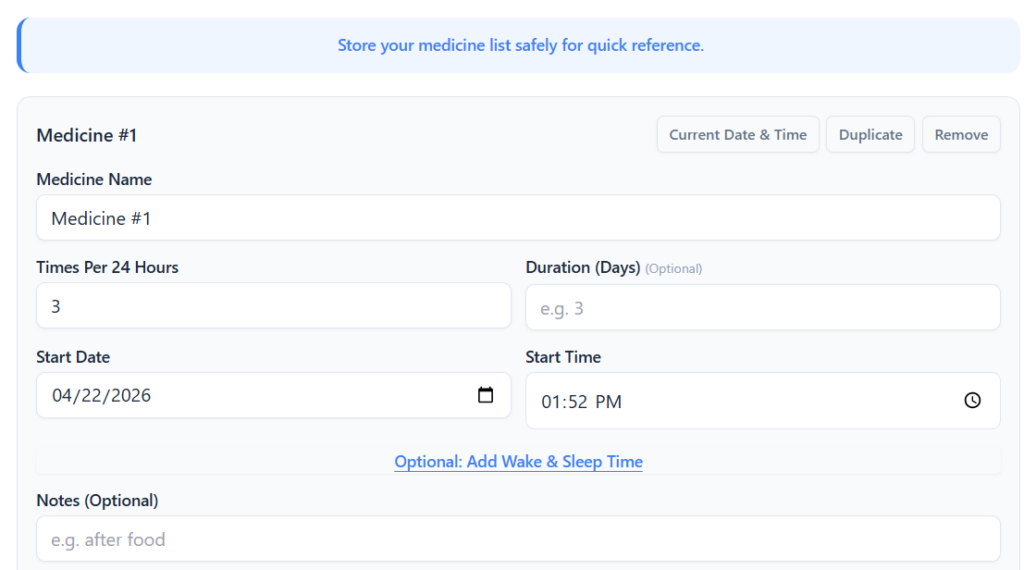
If you take the first dose at 1:52 PM and follow strict 8-hour spacing, the next dose lands at 9:52 PM. The third dose lands at 5:52 AM. This is the point where many people realize strict spacing can push a dose into sleep hours.
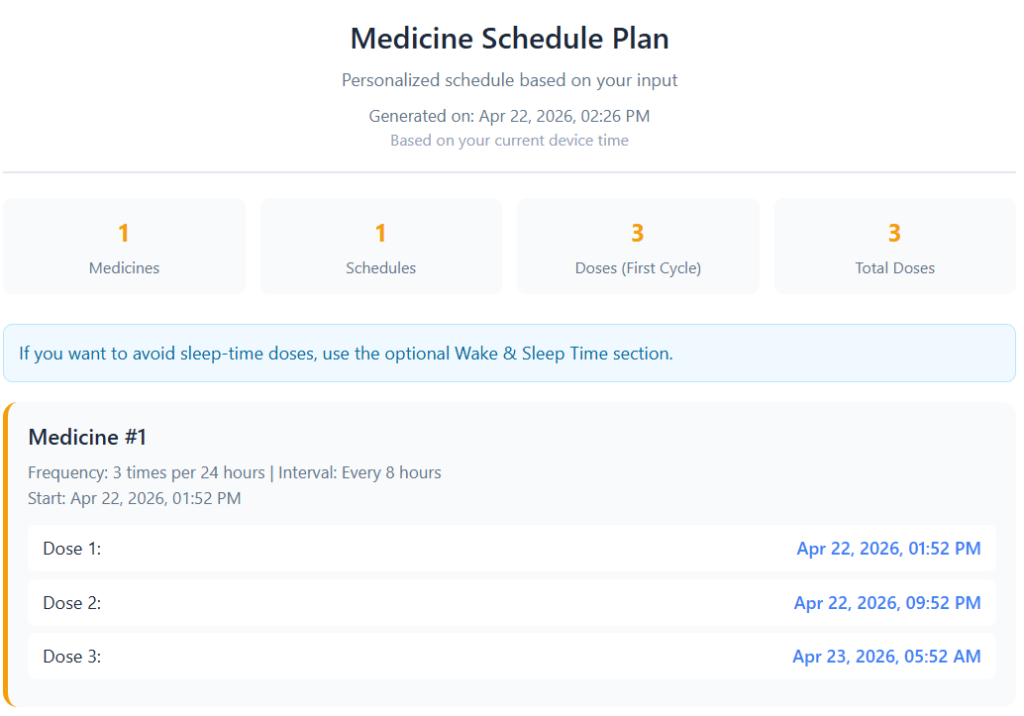
The last dose lands early in the morning. Many people sleep at that time. This is where schedules break down. Some people skip that early dose. Others move the next dose later and “fix” the schedule day to day. Both choices create uneven gaps. That is where mistakes grow.
A safer move is to check the directions first. If the medicine allows flexibility, set the three doses inside your waking hours. If the medicine needs strict timing, keep the 8-hour gaps and use reminders.
Use this medicine 3 times a day calculator to set your start time and get three exact dose times with steady spacing.
Stop guessing and let the times calculate
Manual planning works on calm days. It fails on busy days. People forget the last time they took a dose, then guess the next one. That is how doses end up too close or too far apart. A dose timing tool helps because it removes the mental math.
A practical tool setup usually includes:
- Start time for the first dose
- Wake-up and sleep hours
- Frequency choice, such as 3 times per day
- Support for more than one medicine in one plan
If you use a full 24-hour mode with the same example start time, the tool can produce the same strict set:
- 1:52 PM
- 9:52 PM
- 5:52 AM
That is useful because it shows the true spacing. No guesswork. No missed math. If you switch to a waking-hour option, the schedule can stay inside your day. That is often easier to follow when your prescription does not require strict 8-hour gaps.
Simple reminders also matter. A good plan includes checks such as reviewing each medicine entry and keeping your routine consistent. Small habits prevent most timing mistakes.
Food and sleep can change your best dose times
Medicine timing is not only about hours. Your daily habits affect whether you follow the plan. Food can change how a medicine works. Some medicines need an empty stomach. Others work best with food, or they upset your stomach without it.
Sleep creates another problem. Night doses break routines. A late-night dose can also lead to a missed morning dose. One missed dose can turn into a messy day of uneven spacing.
Tie your dose times to meals when your medicine allows it, because that improves consistency. Avoid night doses unless your label requires strict spacing. Keep the same times each day as much as possible, since routine prevents missed doses.
The small timing habits that mess it up
Most spacing problems do not come from one big mistake. They come from small choices that repeat all week. A person forgets the last dose time, so they take the next one too soon. Another person skips a dose, then tries to “catch up” later with two doses too close together.
Some people shift the times every day based on work or meals, so the gaps never stay steady. A strict plan can fail when someone ignores the night dose and tells themselves they will fix it tomorrow.
Each of these choices breaks the spacing. One slip may not matter much. The real trouble starts when the pattern keeps happening. The medicine stops following a steady rhythm, and the schedule becomes harder to trust. A consistent routine fixes this. It can be strict or flexible, but it needs to stay steady day after day.
If you take more than one medicine
Timing gets harder when you add more medicines. One medicine may require food. Another may require an empty stomach. A third may require exact gaps. If you do not plan it, you end up with overlaps and confusion.
A simple method keeps control:
- Write each medicine and its timing rule
- Note any food requirements
- Place each dose on a single daily timeline
- Check spacing and avoid conflicts
- Review the plan before day one
This takes time once. After that, the plan feels easy.
A calculator helps here because it shows the schedule in one place. It reduces overlap and keeps dose gaps clear.
Missed a dose? Do this next
People miss a dose sometimes. Do not panic when it happens. Your next step matters more than the mistake. Many problems start when someone tries to “make up” the dose too fast.

Take the missed dose if you notice it soon and you still have enough time before the next planned dose. Keep a safe gap before you take the next one. If you realize the miss close to the next dose time, skip the missed dose and return to your normal schedule. Do not take two doses close together unless your doctor or pharmacist tells you to do that.
Some medicines need tighter control. Antibiotics often fall into that group. A pharmacist can tell you the safest move if you feel unsure. That quick check can protect the spacing and prevent side effects.
One missed dose usually does not cause the biggest issue. Repeated missed doses or uneven spacing cause more trouble over time. A steady routine helps you stay consistent and keeps the schedule easier to follow.
A quick check before day one
Before you follow the schedule, do a quick check. Look at the gaps between doses and see if they feel balanced. Ask yourself if you can follow these times on busy days. Confirm the plan matches your prescription directions.
Consistency wins over perfect math
Many people chase perfect timing. They forget the bigger goal. A schedule that you follow every day is safer than a schedule that looks perfect but changes daily. Your body responds well to routine. Your brain also follows routine better than random times. That is why consistency matters more than exact minutes.
When your plan needs a reset
A medicine schedule should fit your life. If it feels hard to follow, adjust it. Pushing through often leads to missed doses and uneven gaps. Sleep changes cause many timing problems. Work shifts, travel, or a later bedtime can push doses too close together. A new medicine can also change the rules. Some doses need food. Some need an empty stomach. Some require strict spacing.
Missed doses and repeat side effects are also warning signs. If you forget the same dose often, or you feel nausea or dizziness after the same dose time, review your timing. Check the label directions again. Confirm if timing must stay strict or if you can place doses within waking hours. Reset your times around your current sleep routine and keep the gaps steady.
